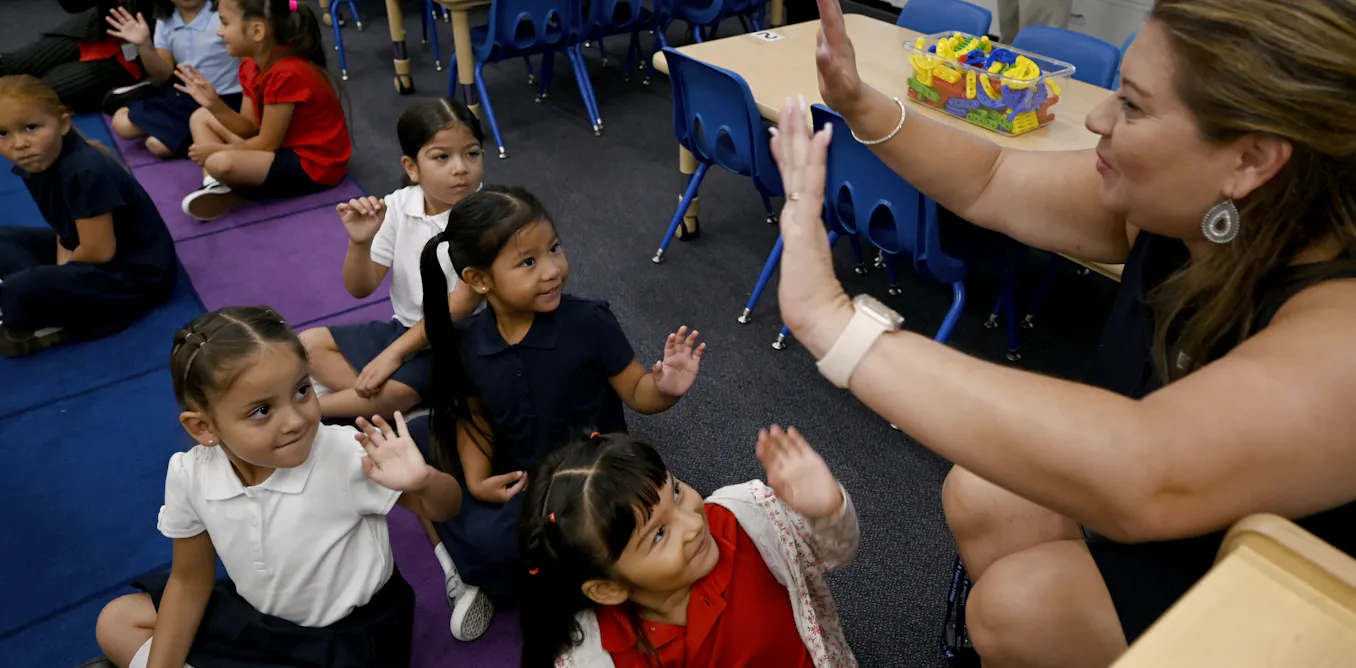While there is a long history of doctor-poets – one giant of mid-20th-century poetry, William Carlos Williams, was famously also a pediatrician – few people seem to know this or understand the power of combining the humanities and medicine.
As a published poet and scholar of the health humanities and ethics, I have a foot squarely planted in each field – or perhaps more accurately, I stand in what I perceive as the overlapping field of healing and poetic practices.
Literature has had a large role in helping me define the kind of physician I strive to be – one who is not only empathetic and a good listener but also a fierce advocate for changing the sociopolitical forces that affect my patients’ lives. I think literature can do this for other health care providers, too.
Narrative competence in medicine
Despite having physicians for parents – or perhaps because of it – initially I had no interest in medicine. It seemed too clinical, too sterile. The work stories my parents shared over the dinner table were intentionally devoid of the personal details that would have interested me.
I was preoccupied with characters in the books I read – who lived in conflict zones, who as children were working instead of playing, who had struggles I couldn’t imagine – and wondered why I had my life and not theirs. What intangible forces shaped their lives in ways different from my own? Now I can directly trace my early infatuation with the written word to my chosen career as a pediatrician and public health researcher.
Narrative medicine is the practice of close reading and reflective writing to build narrative competence. Physician and narrative medicine scholar Rita Charon describes narrative competence as “the ability to acknowledge, absorb, interpret and act on the stories and plights of others.”
Narrative competence, then, could inspire a person to pursue a career in health care and possibly make them a better clinician. In fact, studies of narrative medicine programs have demonstrated that they tend to not only increase students’ empathy and communication skills but also their tolerance for ambiguity and self-confidence. They also improve their open-mindedness, ethical inquiry and perspective taking.
Books introduced me to the breadth and diversity of human experiences and perspectives, as well as to searing inequalities in life outcomes. I wanted to positively change those outcomes in some way – a desire that led me into the arms of medicine, despite my initial misgivings about it.
Using the humanities to address health inequity
Might narrative competence also expand clinicians’ understanding of health disparities and urge them to act in ways that lectures full of statistics couldn’t?
The burgeoning field of critical health humanities theorizes that stories and art can help clinicians understand the unequal realities of different people’s lives and make clinician-patient relationships more therapeutic. It can do this by cultivating clinicians’ awareness of the power differences and structural forces that affect their patients and themselves.
Defining features of this field are collaboration between disciplines – such as between medicine and literature – and a broad understanding of narrative medicine beyond the clinical encounter. Understanding not only human biology but also fields like the history of medicine, queer and disability studies, critical race theory and other forms of knowledge can inform and improve clinical practice.
SDI Productions/E+ via Getty Images
For example, a clinician might turn to research from the social sciences to learn about the experiences of people with disabilities. This could lead her to make her practice more accessible to her patients – an action that would improve equity in health care for people with disabilities.
Before ever meeting my first patient, I gained an expanded knowledge of the diversity of human experience from the books I read. It made me curious about my patients’ stories. And when I felt this curiosity flagging because of stress, exhaustion or burnout, refocusing on the stories seemed to help.
However, medical students are inundated with information about the human body in their training and barely have time to learn about the nonmedical aspects of patient experiences. This negates the fact that disease and health happen in varied and disparate social, cultural and political contexts.
For example, diabetes is a very different illness for a patient experiencing homelessness and racism compared with a wealthy patient who doesn’t experience racism. A patient’s access to resources and their interactions with health care staff affect their ability to get the care they need and the degree to which their basic needs are being met. Rarely are these nuances discussed in a medical school’s endocrinology lecture about diabetes.
Fitting in health humanities education
I believe that physicians must find ways to practice their humanity – perhaps using the humanities – if they wish to be effective healers. But how might they actually do this?
There are ways to fit in more health humanities in all the busyness and bustle of notoriously grueling medical education. As a senior resident, I often distributed poems to my team, printing and posting them above the computers in our cramped hospital workrooms or attaching them to email updates about patient care. Once, during a rare quiet moment in the pediatric ICU, with permission from my colleagues, I read a couple of poems out loud. I remember watching my colleagues’ eyes close and their bodies visibly relax as the words washed over them.
Since then, I have shared poems – my own and others’ – in talks at my institution and across the country. I’ve also led other health care providers in creative writing exercises during workshops, lectures and classes. Many institutions host book clubs, story slams, film screenings and other opportunities for medical learners to engage with the humanities.

The Good Brigade/Digital Vision via Getty Images
While poetry can be intimidating to some, many contemporary poems provide approachable emotional experiences.
Pieces like Safiya Sinclair’s “Notes on the State of Virginia, II” viscerally illustrate how a place that seems innocuous or even beautiful to some can be haunting and traumatic for others.
Monica Sok’s “ABC for Refugees” powerfully paints a portrait of a young child caught between languages and cultures – a reality that many pediatric patients face.
“Ode to Small Towns” by Tyree Daye upends common assumptions about rural life and demonstrates the meaning of place in hymnlike vernacular.
In “Medical History,” Nicole Sealey shares a many-layered patient perspective on a part of health care that, for many of my students and colleagues, has been reduced to a series of check boxes on a computer screen.
These and other poems – not to mention short stories, novels, personal essays, films, podcasts and comedy shorts, among other genres of storytelling – provide fertile ground for enhanced understanding of the human condition, as well as inspiration for a clinician’s own potentially transformative reflective writing.

This article is part of Art & Science Collide, a series examining the intersections between art and science.
You may be interested in:
Melding literature and medicine
The possibilities for collaboration between literature and medicine are wide open. In a country that spends more per capita on health care than economically similar nations yet continues to have extreme inequalities in outcomes, it’s clear that the U.S. needs to do things differently.
I believe all clinicians have a role in recognizing and grappling with how everyone has been shaped by an inequitable society. The history, sociopolitical context, imaginative perspective and reflective practices the humanities offer may improve the practice of medicine.
Through understanding others’ experiences and reflecting critically on their own, every clinician can move closer to being the kind of healer they intend to be.
The article Why the humanities are needed in health care by Irène Mathieu, Assistant Professor of Pediatrics, University of Virginia was published on 05/01/2024 by theconversation.com

















![Our Malaysian Camper Adventure: A DISASTER Unfolds! [S11-E7] Our Malaysian Camper Adventure: A DISASTER Unfolds! [S11-E7]](https://i.ytimg.com/vi/1sbBiEXpe6Y/maxresdefault.jpg)